I Found a Neurologist Who Gives Me Hope

A broken promise can often lead to immense disappointment. For someone with myasthenia gravis (MG), a failing immunosuppressive medication can easily lead to a broken heart.
Immunosuppressive medications combat the autoimmune nature of MG. Unfortunately, I have refractory seronegative MG. Refractory means that either I do not respond to treatment or the side effects of said treatment are too severe to justify long-term use. Seronegative means that specialists haven’t identified the antibody responsible for disrupting the communication between my nerves and muscles.
In other words, specialists don’t know what is responsible for my MG.
It took four years of searching, including 18 months of chemotherapy (cyclophosphamide), to find the right immunosuppressive medication for me. You can imagine my surprise and delight when my condition improved a few months after I started a new immunosuppressive medication called cyclosporine. For the first time, my medication was working, which meant fewer hospitalizations, no more chemotherapy, and easier breathing. I was ready to take on the world!
Sure, I was experiencing some side effects, but that was a small price to pay for better health in general. The side effects were worth it because I had something that I hadn’t had in a while: hope.
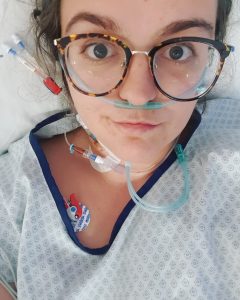
(Photo by Retha De Wet)
After about 18 months of cyclosporine, my symptoms started to flare again. My voice was soft and breathy, my legs were wobbly, and my neck was floppy.
It was happening again.
The panic sank in.
I tried to make an appointment with my neurologist, a renowned professor in neurology. But the earliest appointment I could get was in five months, which I knew would be too late if I were relapsing.
Over the next month, I deteriorated seriously and rapidly. Even my breathing was severely affected. My mother decided to contact my neurologist from my hometown. When she heard about my troubles, she urged me to come to her hospital. I was admitted to the ICU as soon as she saw me.
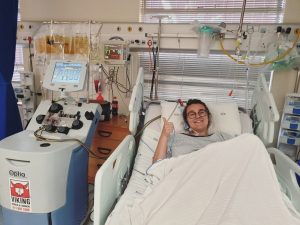
(Photo by Retha De Wet)
That was when I received my first sessions of plasmapheresis. The initial session was terrible and filled with severe nausea and vomiting. However, after the second and third sessions, I began to improve.
Even better, I found something that I had lost once again: hope.
Following that hospitalization, I returned to the neurologist, who was a two-hour flight away. My MG is not stable, and I am not functioning optimally, but I can rest assured that my neurologist will take care of me if I experience another MG crisis.
Despite being admitted to the ICU twice in the past four months, my neurologist made sure that I continued my studies. I am proud to say that I have officially completed my degree and am a speech-language pathologist.

(Photo by Retha De Wet)
I have decided to relocate to my hometown next year so I can see a neurologist who gives me hope. I don’t know what the future of my treatment holds, but I know that my neurologist will ensure that my quality of life is considered every step of the way.
Never stop fighting. Life is beautiful.
***
Myasthenia Gravis News is strictly a news and information website about the disease. It does not provide medical advice, diagnosis or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website.







Shannon Talerico
Reading your story brought me back to the years I first began my journey with MG.
I was only 14 when the symptoms began. Double vision, severe headaches, fatigue were the first ones. Our family doctor at the time had decided I had a brain tumour .... well, needless to say we were devastated ! The thing was that the doctor only took a blood test and nothing else. So my dad sent me to his doctor who in turn sent me to a neurologist in Calgary, AB (I’m in Canada).
After one day of some exhausting tests. I was diagnosed with MG. So rare that most of the medical team had only read about it in medical journals. But the most surprising was my age. I was the youngest at the time to ever be diagnosed with MG.
My neurologist, Dr. Maryanne Lee, had been treating MG patients for some time.
There were new trial treatments out that I became a part of, with success. It was a 4 year long, challenging, emotionally painful journey but I went into remission. I had a combination of treatments; meds; Mestinon, immuran, prednisone. I had many crisis through out. Not able dress myself, do my hair, walk, slurred speach, choking when swallowing, droopy eye lid, extreme whole body weakness, zero immune system, I’d catch a cold in seconds then by end of day it was pneumonia. I had a respiratory crisis and stopped breathing. Woke up days later breathing by a machine. From there treatment went to plasma exchanges, thymectomy and same meds. I had started to get better, longer times between flare ups to eventually weening off the meds to no meds. But the one thing that made all the difference was Dr.Maryanne Lee. I was so depressed, scared, and lonely. Aside from my family I had very few friends left that understood. Teachers thought I was on street drugs or drunk when I went to school. So after all the treatment they could do, Dr. Lee said to me “Shannon, it is your turn now. You get to decide if you want to live or die by letting this disease take control again or fight it. You have to put mind over matter, change your thinking to positive and gratitude. “
So, I did. I am 48 now, I was married, had a beautiful daughter, and I’ve had very few flare ups, and when I did they were minor. I controlled it with rest and self love.
Your medical team, your support from family and friends are extremely important; but the most is yourself.
I wish you so much love and success !!
Aubrey Shelton
My name is Aubrey Shelton...i live in Charleston (hurricane) WV...i have been diagnosed with mg for about 3 yrs now.;everyyhing that u just described about yourself is a mirror of myself as well..i have been through it all..and fast...im 43 yrs old... symptoms started at age 39!Took almost 2yrs yo diagnose me!!Im still having a very difficult time!!No work..no disability..no quality of life!!!Ive done plasma exchange 4x..IVIG WAS GREAT.. ONCE A MONTH..BUT i don't have good insurance..i get Medicaid..so IVIG isn't covered anymore!!I just wanted to thank you for your comment because you really gave me something i haven't had too much of..and that is hope and im grateful.Thank you
Dr.Patricia Anderson
I am a 68 yr old retired female Doctor diagnosed with MG 2.5 yrs ago. I have been on Mestonin, Prednisone, Cellcept and IVIG. Recently had to stop ivig due to horrible pain. I've been told not to take vaccine but I have serious concerns over this. Also prior to diagnosed I was on Beta-Blockers for high blood pressure now being off these I am even more concerned over my blood pressure
Joan Medi
Dear Dr. Anderson
Your story is similar to mines. I was diagnosed a year and a half ago. Had two very bad episodes that put me in the ICU. I’ve used Mestinon, IVIG,
Imuran, Cellcept and was also taking a blood thinner to regulate my heart beat. I’m no longer taking those meds. Now I’m taking a new medication called Soliris. So far it seems to be working. The side effects are very minimal. Hoping this medication could work for you as well. Take care be safe
sue bowen
Hi just to let you know I am 70 years old and had MG for 56 years (WOW ) and have an amazing life despite the ups and downs of having this diagnosis . All those years ago little was known and very little treatment was available . So stick with it and kive the beat kife you can despite MG
Love and beat wishes
Elsie
Dear Retha, can you tell me who is the neurologist you went to. I’ve been diagnosed with MG, but need a second opinion on my meds.
Kind regards
Barb Nelson
I was diagnosed with Myasthenia Gravis when l was 14. I had a thymectomy at 15 and very quickly got tired of visits to the hospital to visit the specialist and wait hours for medication so l stopped taking the mestinon.Thirty years later l was still well and still medication FREE.l studied to be a teacher, travelled the world , married and had two children. In my late 40's ,after a long period of stress the symptoms began to rear their ugly head. After treatment with immuran l have now had another 20 years of good health. I conduct walking groups, swim and go to the gym.life is sweet----- NEVER GIVE UP!
Anna
My daughter at 27 diagnosed with MG, now on and off for 2 years. Need not to say further you know how I feel. Very heart broken. May I know who is your treating doctor, my daughter has been advised to IVIG and I am sceptical about this and like to consult for second opinion. Who prescribed Solaris? I would really appreciate any good doctor you experienced with a referral. Thank you so much! Anna
Linda Adams
I’m desperate and scared to death. I’m a 72 year old woman who has had so many ups and downs for years having diagnosis of RA, fibromyalgia, every arthritis disease there is spine, back, neck problems then double vision I fought with for a year or more finally sent to an eye specialist in thyroid eye disease and he found my diagnosis of myasthenia gravies I live around the Tulsa, Oklahoma area and I have been trying to find a neurologist desperately for 4 months seems they all died retired or quit my neck is getting so weak and I’m so tired and weak getting hard to swallow solid food. Can someone please help me find a neurologist that will take Medicare and a 72 year old woman who is ready to give up yet I’m a fighter and life is too precious. I’m an actor in front of my family but my acting is fading and they see how I’m struggling. I have 3 beautiful great grandchildren I want to see graduate they aren’t even in real school yet lol. I have to beat this but I can’t do this on my own is there any neurologist in the Tulsa, Oklahoma area that can and will take on a real challenge like me. Today is October 20, 2021 my 72nd birthday
Amy Saunders
Hello there! It was really nice of you to explain just how fortunate we are these day because the way we treat brain issues have significantly improved thanks to the latest technologies. I think that's why I'll have to ask my uncle to book an appointment as soon as possible so he can recover from his health problem. Since last week, he's been throwing up non-stop due to this severe headache he had and I feel really bad for him. //www.ntnsc.com/