Abnormal Electrical Activity of Neurons May Be Biomarker of Juvenile Myasthenia Gravis
Written by |

The interval between two electrical impulses in neurons correlates with clinical severity and may be a biomarker of juvenile myasthenia gravis (JMG), according to a small study.
The recent research, “Serial Stimulated Jitter Analysis in Juvenile Myasthenia Gravis,” was published in the journal Muscle & Nerve.
JMG patients whose disease begins before puberty are more likely to achieve remission than adult patients, but these periods of improvement may be followed by relapses. Unlike adult patients, those with JMG still lack studies on electrophysiological (the electrical activity of neurons) outcome measures.
The team from Emory University assessed disease activity in JMG patients using serial stimulated jitter analysis (Stim-JA), which was correlated with clinical severity stage using the Myasthenia Gravis Foundation of America (MGFA) classification system.
Jitter is the normal variability in the interval between two action potentials, or electric impulses, in each motor neuron — cells that control muscle contraction.
The 13 patients (nine girls, four boys) had generalized MG (muscle weakness and fatigue not confined to the eye muscles or other specific muscles) and were acetylcholine receptor (AChR) antibody positive, a MG hallmark. Mean age was approximately 13 years (range 5-19 years).
They were followed-up every three to six months between 2014 and 2017 (mean follow-up duration 25.3 months) in a multidisciplinary pediatric MG clinic at a tertiary care children’s hospital. The staff included a pediatric neurologist, a pediatric physical therapist, and a pediatric pulmonologist.
Besides disease duration and severity, the researchers also collected data on type of management — immunomodulatory therapy or thymectomy, a common surgical procedure in MG to remove the AChR-producing thymus gland — Stim-JA values, and bilateral grip strength (using a hand-held device called a dynamometer). Pulmonary function also was assessed in a sitting position in patients aged 5 and older.
Six patients (43%) showed bulbar muscle weakness — which may affect speech, swallowing or chewing — and respiratory manifestations at the initial visit. Average JMG duration was nearly 4.4 years and average onset age was 9.5 years
The patients received diverse treatments, including Mestinon (pyridostigmine, 100%), steroids (85%), the immunosuppressive azathioprine (38%), intravenous immunoglobulins (or antibodies, 92%), Rituxan (rituximab, 8%), plasma exchange (23%), and thymectomy (54%).
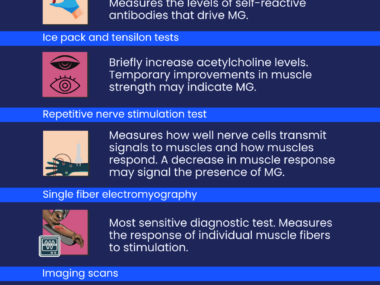
All 13 patients underwent at least two Stim-JA assessments of the right orbicularis oculi muscles, which closes the eyelid, with a mean interval of 10.3 months.
The results revealed abnormal (increased) Stim-JA values at both baseline and at follow-up. Although there was no statistically significant difference between baseline and follow-up, the researchers noted an improving trend with treatment. Patients with refractory (treatment-resistant) JMG or with clinical relapse demonstrated persistently abnormal jitter values
Also, unlike respiratory function and grip strength, the Stim-JA data correlated with clinical severity. This link between jitter values and clinical assessment was useful in directing treatment, the scientists noted.
Overall, the results showed that “stimulated jitter values are sensitive biomarkers of disease activity in JMG,” the researchers wrote.
Among the study’s limitations, the scientists mentioned the small sample size and the lack of standardized MG outcome measures.

Cortie Potter
Thanks for the information on M/G in children.. I am a patient with M/G. ,have been doctoring for 10 years .. My body shut down, couldn't talk , swollow, eat. walk spit no energy, droopy eyes etc. I am 89 yrs. old. take gamma gard once a month, mestion, cellcept , and lots of vitimans. Have little energy. on walker and wheelchair.. have lots of bad days. Guess I am doing good to be alive.. Heart trouble and pacemaker. oxygen..