Videos: Rare Takes
In this video series, Friedreich’s ataxia experts discuss important topics related to diagnosing, managing, and treating the disease, from the importance of early diagnosis to collaboration with patients, families, and other providers.
Latest News & Research
In this guide
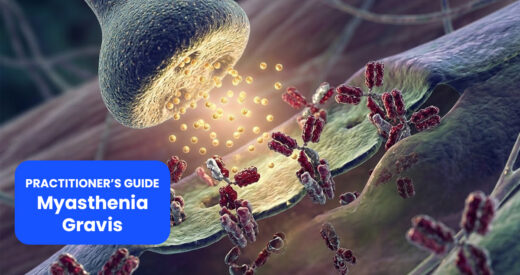
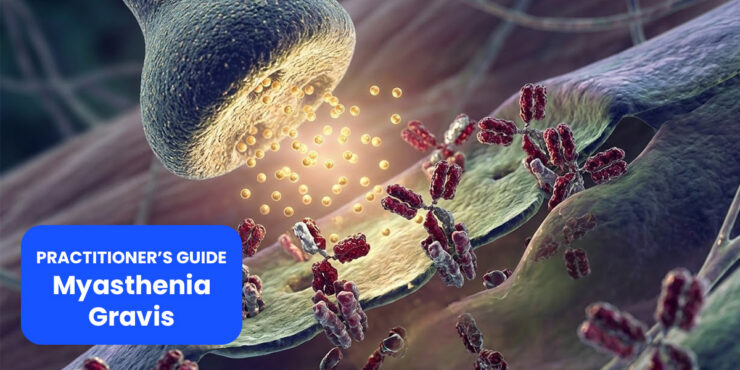
Myasthenia gravis (MG) is a chronic autoimmune neuromuscular disorder characterized by varying degrees of skeletal muscle weakness and abnormal fatigability. Although relatively rare, MG has been studied extensively as a prototypical antibody-mediated autoimmune disease, providing crucial insights into neuromuscular transmission and immunopathogenesis in multiple neuromuscular diseases.

Myasthenia gravis (MG) is an autoimmune neuromuscular disorder characterized by fluctuating, fatigable skeletal muscle weakness due to impaired neuromuscular transmission. Accurate and timely diagnosis is critical, as early intervention improves outcomes and prevents complications such as myasthenic crisis.

A defining feature of MG is the presence of serum autoantibodies targeting critical components of the neuromuscular junction (NMJ). Traditionally, MG was classified simply as ocular versus generalized, but modern approaches integrate antibody status with demographic and thymic features.

Thymic abnormalities, including thymic hyperplasia or thymoma (a slow-growing tumor composed of neoplastic thymic epithelial cells and non-neoplastic T lymphocytes) are common in MG.

Pharmaceutical and other treatments for myasthenia gravis (MG) can improve symptoms, reduce autoimmune attack, and prevent complications such as myasthenic crisis. Treatment selection is guided by antibody subtype (AChR, MuSK, LRP4, or seronegative), disease severity, and individual patient factors.