Gut Microbes, Metabolic Changes May Provide Accurate MG Biomarker
Written by |
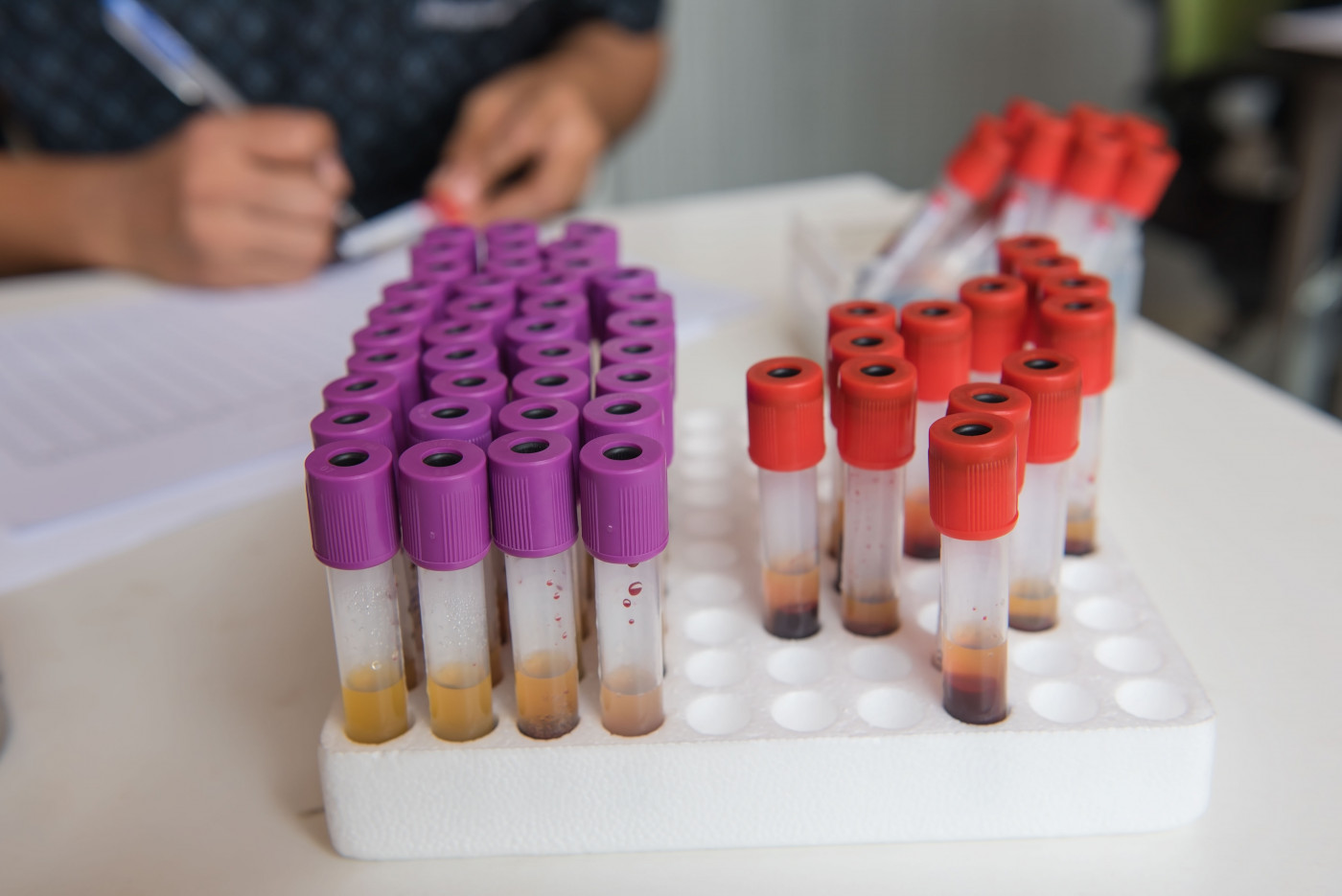
Analyzing microbial and metabolic changes in fecal samples may provide a highly reliable way to diagnose myasthenia gravis (MG) and monitor its severity, according to a new study in patients and mice.
The research, “Perturbed Microbial Ecology in Myasthenia Gravis: Evidence from the Gut Microbiome and Fecal Metabolome,” appeared in the journal Advanced Science.
The gut microbiome — the community of bacteria, viruses, and fungi — plays a key role in maintaining immune function and has been implicated in diverse disorders, such as stroke, epilepsy, and Parkinson’s. Specifically, immune dysregulation via alterations in the gut microbiome has been suggested as a driver of multiple sclerosis and other autoimmune diseases, but evidence in MG is still lacking.
Aiming to address this gap, a team from Chongqing Medical University, in China, and SUNY Upstate Medical University compared the gut microbiome of 70 symptomatic MG patients (39 women, mean age 46 years, disease duration 5.7 years) with that of 74 healthy controls.
To have a complementary assessment of microbial activity, the scientists also employed a technique called gas chromatography‐mass spectrometry, which enabled the analysis of metabolic changes (metabolomics) in fecal samples.
The results first showed that the patients had reduced diversity in their gut microbial species, which correlated with the quantitative MG score of disease severity. The lower the diversity, the greater the severity, as illustrated when comparing patients to those without history of respiratory crisis.
“These findings highlight that microbial diversity indexes may provide a novel clinical tool for assessing MG severity,” the researchers said.
Then the data revealed that the gut microbiota composition was significantly different in patients and controls, but not when comparing men with women or different disease subtypes. The difference between patients and controls was driven by 80 bacterial operational taxonomic units (OTUs) — clusters based on genetic sequencing — which primarily belonged to the phyla (a level of classification between kingdom and class) Firmicutes, Bacteroidetes, and Actinobacteria.
The altered microbial composition was associated with fecal metabolic changes, with 30 metabolites being responsible for differentiating patients from controls. Most of these metabolites were involved in amino acid, nucleotide, and microbial metabolism. Amino acids and nucleotides are the building blocks of proteins and DNA/RNA, respectively.
A subsequent analysis found that 38.75% of the altered bacterial OTUs were linked to changes in more than one metabolite (product of metabolism). Also, some microbial OTUs were slightly associated with gender, anxiety, long-term immune therapies, disease duration, thymus hyperplasia (enlargement), and anti-acetylcholine receptor antibodies.
Nineteen OTUs, mainly from the Lachnospiraceae, Erysipelotrichaceae, and Bacteroidaceae families, strongly correlated with MG severity.
An assessment of OTUs and metabolites with differences in MG patients then demonstrated that a combination of four OTUs belonging to the Clostridiaceae, Lachnospiraceae, Erysipelotrichaceae, and Bacteroidaceae families, and six metabolites — leucine, cytosine, oxalic acid, N‐Acetyltryptophan, d‐Glyceric acid, and xanthine — had 100% accuracy in differentiating patients from controls.
To study whether an impaired gut microbiome may contribute to the onset of MG, the investigators subsequently used a germ-free mouse model of the disease, colonized with MG or healthy microbiota.
Four weeks later, the mice receiving MG microbiota showed significant locomotion impairments. This effect could be reversed if using both MG and healthy microbiota, “suggesting that the gut microbiome may contribute to the development of MG,” the investigators said.
In line with well-known disease-related alterations, the mice receiving MG microbiota also showed increased gut and serum levels of the inflammatory molecules TNF-alpha, IFN-gamma and IL-10. As with the altered locomotion, use of healthy microbiota reversed these changes. Further analyses of the gut microbiome of these mice found similar changes as those observed comparing patients to controls.
“Foremost in this study, we found that the combination of fecal microbial and metabolic markers can discriminate the MG subjects from healthy controls with an astonishing 100% accuracy, highlighting the potential of this approach as a novel diagnostic biomarker of MG,” the scientists said. “Our findings provide new avenues by which to enhance our understanding of MG pathogenesis, and to develop novel diagnostic and therapeutic tools for MG.”



Jorge
So what can we do to our gut to help with our MG