The Cost of Uneducated Care
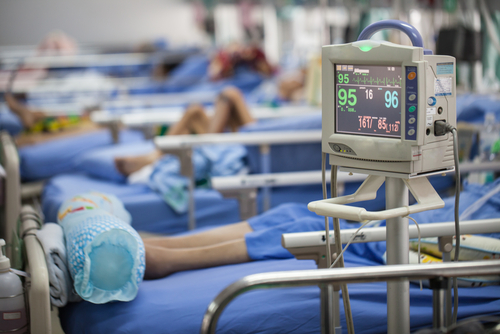
During my most critical year with myasthenia gravis, I spent an inordinate amount of time in the emergency room and on various hospital floors. A good deal of the ER staff soon got to know me by name and, while clueless as to how to help my rare but potentially deadly disease, they were often kind.
Their kindness aside, the hospital was a constant place of tumult, chaos, and fear. I was never able to rest and trust that the practitioner, nurse, respiratory tech, and others knew how to assess me properly and the unfolding situation, would offer me critical medications on time, or would offer me safe medications that wouldn’t throw me into yet another crisis.
It looked like a never-ending school day in which you teach and reteach the same material to a rotating group of students who you are keenly aware are not really getting it. Every flush of the IV, every med round, and every ordered test begs the question of what and why, demanding deeper analysis as a barrier from mistakes — mistakes I would ultimately pay a high price for.
That first year taught me a lot about medicine I never wanted to learn. Each crisis instilled in me a growing fear of the men and women meant to save me who would doubt, criticize, or blame me as they failed to understand the gravitas of what they were treating.
It was not until my first ER trip to another hospital a couple of hours away, where my MG specialist rounded, that I got my first taste of security. I remember the frantic two-hour drive being compacted to a mere hour and a half with my frenetic mother behind the wheel, desperate to get me real help. I could not go back to the hospitals near me, so bad was the trauma I experienced under them.
We rushed into that quiet ER and checked in at the registration desk as usual. As soon as they heard “myasthenia gravis,” they immediately took me back. Within 10 minutes, I was assessed by nurses and an ER physician who not only believed me but also expressed concern. They said they would be sending me to the neurology floor immediately for observation. I reached the floor, unsure of what was to come next. And that is what I have learned is so innate to our experience in rare diseases and chronic illness like MG — being unsure of the next moment, the next encounter. It is hard to be brave when we are always faced with a measure of uncertainty.
I found the unit to be fully and wonderfully trained in MG protocols by specialists, and once I realized that I didn’t have to explain anything for the first time since my diagnosis, I could actually rest. I could rest in the care of the team around me and the choices being made, and I wept gratefully.
How badly do we all need the feeling of rest and security in our medical encounters? How often do we long to be able to have the care we desired and not what we encounter?
I pray security becomes the rule rather than the exception. I wonder how it would change for patients like us if medicine met us where we were and allowed us to rest.
***
Myasthenia Gravis News is strictly a news and information website about the disease. It does not provide medical advice, diagnosis or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website.







Comments
dorothy smith
My hospitals the bill exactly.
JOHN D AUTORE
Your story and comments are so "RIGHT ON THE MONEY !!!" I took me 8 months, many CIGNA HEALTHCARE referrals, and two hospitals to get a REAL Diagnosis for my weakening condition. I had MYASTHENIA GRAVIS ... but not a single doctor .... including two consulting Neurologists ... at the first hospital ...of three hospitals .... from Feb 4-27, 2020 could diagnose me. Instead I got three types of PNEUMONIA, acute respiratory failure, a collapsed right lung, 4 months of breathing tubes, and a TRACH .. before a knowledgeable floor nurse at the second of 3 hospitals, recognized all my 8 or 9 symptoms and diagnosed me on the spot. " I know exactly what you have. We have patients right here at St. Joseph's that have all the symptoms that you have. YOU HAVE M.G. " Almost every other doctor was clueless .. in spite of my 8 or 9 ACCURATE SYMPTOMS........ One cardiologist even wrote me up as a "DIFFICULT HISTORIAN" I told the truth !!!! and every symptom was CORRECT and all from only a single disease. I was SO HAPPY to finally see an M.G. doctor ... who knew what M.G. was !!!! and did not look at me weirdly. I had waited 8 long months and got sicker and weaker.....and lost 43 pounds. I probably lost much more ... as they would not let me eat and swallow real food for three months ... until I pasted the Oreo cookie ( camera up your nose to watch your swallowing) test. They finally let me start eating real food ... even if it was hospital food .... and have have regained some weight .... but my muscle tone wasted away from 4 months stuck in a hospital bed and shitting liquid/paste mustard condensed soup poop all over my crotch every day. I proudly hear an engraved MYASTHENIA GRAVIS wristband ... so the next clueless doctor .... can read it ... and KNOW ... in case they sedate me and fill me with IV tubes, unnecessary hoses, PNEUMONIA, and three body holes again before shipping me off to a second hospital UNDIAGNOSED.....